
A prescription is an order written by a licensed healthcare professional, such as a physician, allowing a patient to receive a specified medication for a health condition. Some prescriptions are handwritten on paper prescription pads. Most are transmitted digitally, using information from the electronic medical record to streamline the process.
Table of Contents Add a header to begin generating the table of contentsIn the United States, the dispensation of certain drugs is regulated by the Food and Drug Administration (FDA). These drugs are known as prescription medications because they can only be obtained by consulting a prescriber first. Prescription medications are classified as Rx-only.
Some prescription medications have a potential for misuse. These medications are classified as Schedule I – Schedule V. Schedule I medications, such as heroin, are illicit drugs considered to have no therapeutic value. They cannot be prescribed. Schedule II drugs are considered to have a high risk of misuse; these drugs are closely monitored but have therapeutic value that outweighs the risk in some cases. Examples of schedule II drugs are Adderall and oxycodone. Rx-only drugs that don’t fall under Schedule I – Schedule V have not been identified as carrying a risk of misuse. Note that a drug’s schedule only categorizes its potential for misuse and does not represent all aspects of its safety profile. Some drugs are available without a prescription, over the counter or, “OTC”.

In the United States, medical doctors (MD/DO), dentists (DDS/DDM), physician’s assistants/associates (PA), and nurse practitioners (NP) may write prescriptions. While pharmacists (PharmD) are not prescribers in the majority of states, they may prescribe from a limited list of medications in some states. Only providers with a Drug Enforcement Administration (DEA) number can write prescriptions for controlled substances from Schedule II – Schedule V, which are drugs with a potential for misuse.
An Rx number is used by the pharmacy to keep track of a prescription. Every prescription gets a unique Rx number from the pharmacy. For example, if a patient receives a three-month supply of bupropion 150mg with no refills and then returns to the doctor 3 months later and receives a second prescription of bupropion 150mg, they will have separate prescription numbers, despite the second prescription being nearly identical. These separate numbers allow the pharmacist to search individual prescriptions and accurately track refills and changes in dosage and instructions that may happen over time.
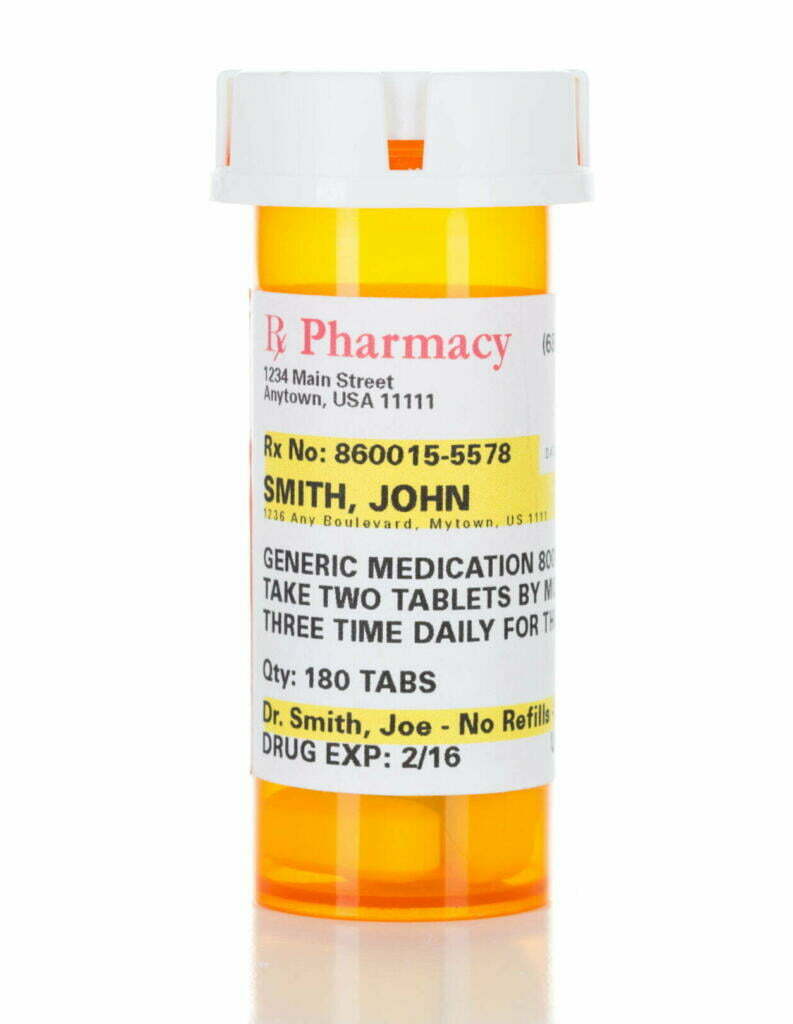
While we may not realize it, medication errors are still a big issue that the healthcare industry faces. The only way to combat errors is to make sure every prescription is written in the same format.
Medication errors are very costly both monetarily and in patient morbidity and mortality. The statistics are alarming, and medication errors remain a major reason why malpractice insurance is incredibly high for healthcare practitioners. Learning early on how to check and recheck prescriptions can decrease a lot of stress for both patients and practitioners. Every detail of the prescription matters. For example, writing the patients identifying information prior to signing the prescription is important if using a written pad, as losing a signed prescription with no name can be dangerous if it falls into the wrong hands.
A prescription MUST include the following:

In this example, the patient, Irma Juror, will be able to use their date of birth and address to verify their identity with the pharmacy. They have been prescribed Metformin in 500mg tablets. The patient has been instructed to take 1 tablet by mouth every day with their evening meal. Prescriptions are typically written in 1-month or 3-month supplies. In this case, the patient is given a 1-month supply of 30 tablets and two refills, so they will have enough medication for three months before they need to visit their prescriber again. The quantity is sometimes written with a # sign before it to differentiate it from other numbers on the prescription, such as the strength. They may also be able to request refills electronically or over the phone, either through their doctor’s office or through the pharmacist, who will contact the doctor’s office for them.
While this can feel very daunting as a medical student and new resident physician, after a bit of practice and consistently following the steps above, it will feel easy and natural. Especially with the predominant way to prescribe being via the computer, there are systems in place to double-check prescriptions and ensure there are no contraindications between the patient’s home medications and the new medications being prescribed.
To get more information on the signature (sig) codes that practitioners use to abbreviate their prescriptions, read below!
| ad | right ear |
| APAP | acetaminophen or Tylenol - short for N-acetyl-p-amino-phenol |
| as | left ear |
| au | both ears |
| bid | twice a day |
| cap | capsule (cannot use interchangeably with tablet) |
| DAW | dispense as written - if written for a brand name medication, indicates that the generic version may not be substituted |
| DEA | drug enforcement agency - some prescribers have a DEA identification number that allows them to prescribe controlled substances |
| gtt | drop |
| NPI | National Provider Identifier - a unique 10-digit identification number for healthcare workers |
| od | right eye |
| os | left eye |
| ou | both eyes |
| po | by mouth |
| prn | as needed |
| q4h | every 4 hours |
| q6h | every 6 hours |
| qd | every day |
| qhs | every night at bedtime |
| qid | 4 times a day |
| qod | every other day |
| sc | subcutaneously |
| sig | directions |
| tab | tablet (cannot use interchangeably with capsule) |
| tid | three times a day |